More than systems or technology, it’s clinicians who define the quality of care. Your unwavering efforts, whether diagnosing complex cases, performing delicate procedures, or simply listening to a patient’s concerns, shape every outcome. When things go well, the credit belongs to your skill and judgment. Yet, when outcomes fall short or patients feel dissatisfied, physicians often bear the weight, regardless of intent or effort.
Nothing weighs heavier on a provider’s mind than the threat of a malpractice lawsuit. Beyond paperwork and courtrooms, it’s the anxiety of having your reputation questioned, your years of training overshadowed, and your livelihood put at risk. Even unfounded claims can drain finances, disrupt patient care, and cause lasting emotional stress.
As a provider, the last thing you want is to be pulled into a legal battle that can cripple momentum and hinder long-term growth. The wiser move is to stay ahead by proactively managing malpractice risk. It’s about anticipating risks, instilling the right safeguards, and building systems that protect your practice. In light of this, let’s examine the most common physician errors that drive malpractice claims and the proven best practices you must adopt to minimize risk and address vulnerabilities before they escalate.
Medical malpractice is a reality every healthcare provider must acknowledge. According to the National Practitioner Data Bank (NPDB), there were 11,601 malpractice payment reports in 2024, and approximately 4,722 in the first half of 2025 alone. These numbers make it clear: malpractice risk remains a significant concern.
Even the most skilled providers aren’t immune to risk. Identifying the errors that often lead to litigation is critical to protecting your practice and your reputation. Here’s a closer look at the missteps that frequently put clinicians in jeopardy of malpractice claims:
Medical errors may top the list of malpractice triggers, but often, even small, overlooked details can land providers in hot water. The upside is that most of these risks can be prevented.
Integrating the following best practices into your workflow keeps your patients safe, reduces errors, and shields your practice from costly malpractice claims.
At the heart of every physician’s oath is a commitment to patient safety and excellence in care. Patient safety is a non-negotiable principle that must be embedded into every decision, procedure, and interaction. Implementing robust safety protocols, such as standardized protocols for patient identification and medical procedures, helps catch potential risks before they escalate into serious problems.
Equally important is staying current with healthcare regulations, including updates to malpractice statutes, patient privacy rules, and electronic health record standards. Proactively integrating new protocols and addressing emerging legal considerations ensures that your practice remains compliant and enhances overall patient care. A strong safety culture combines effective protocols, regulatory awareness, and proactive risk management, forming the bedrock for malpractice risk management.
Many malpractice claims don’t result from medical errors, but from patients’ frustration or dissatisfaction with communication and the physician-patient relationship. According to the recent Candello report, about 30% of all claims involve communication failures.
Clear, consistent communication is the strongest defense against malpractice claims. To protect your patients and your practice, focus on these essential elements:
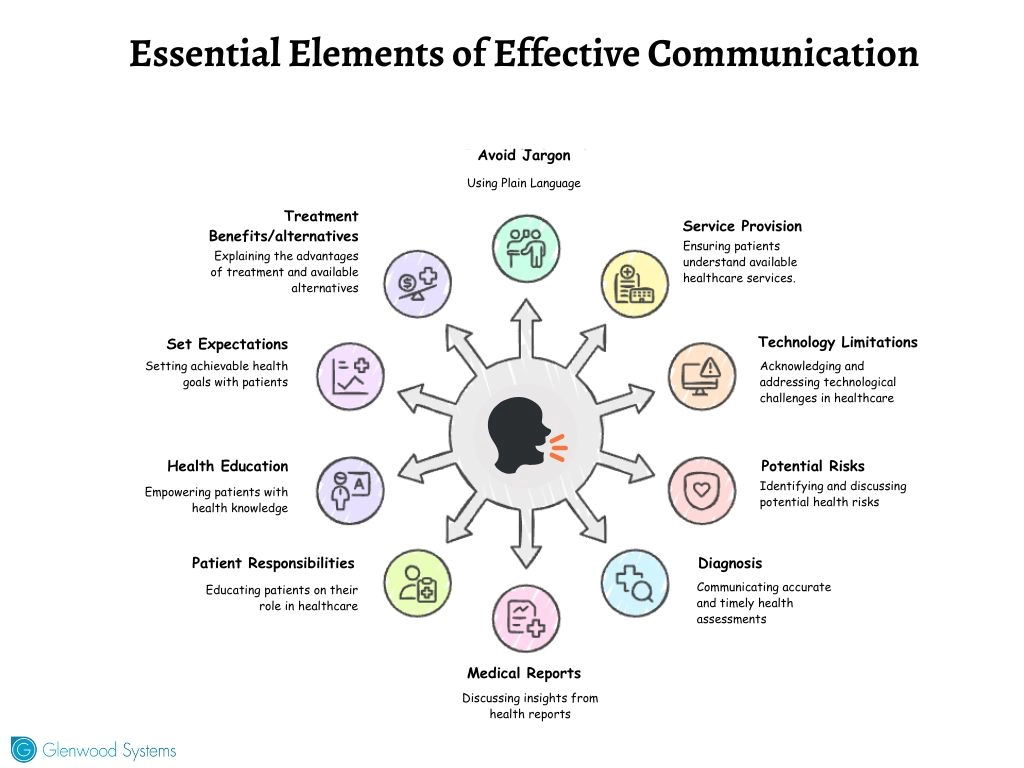
Essential Elements of Healthcare Communication
Healthcare professionals who prioritize patients’ emotional concerns alongside medical care decrease their exposure to malpractice claims.
Robust documentation is like a shield for providers against malpractice risk. However, documentation gaps increase the chances of an indemnity payout by more than 100%. According to Candello’s 2024 Benchmarking Report, which reviewed over 65,000 malpractice cases closed between 2014 and 2023, 1 in 5 cases involved documentation failures.
The most frequent and high-risk documentation errors include:
The American Academy of Family Physicians (AAFP) recommends an updated approach to documentation using the SOOOAAP note format, an enhanced version of the traditional SOAP note. SOOOAAP stands for Subjective, Objective, Opinion, Options, Advice, Agreed Plan, and emphasizes clarity, accuracy, and patient-centered care. Here’s a brief overview of each component:
The SOOOAAP format provides a comprehensive legal safeguard, ensuring that every step of the care process is handled with diligence and transparency.
When your team isn’t aligned, errors are more likely to occur. Consistency across your team is pivotal to mitigating malpractice risk. Every member of your practice, including physicians, nurses, medical assistants, and administrative staff, must follow the same protocols and standards to ensure safe and high-quality patient care.
Implement regular team meetings to review workflows, address challenges, and reinforce best practices. Establish shared policies and clear responsibilities so everyone understands their role in patient care. Standardize procedures to reduce errors caused by assumptions, miscommunication, or missed steps. Moreover, encourage a culture of accountability and collaboration in which team members feel comfortable speaking up if they notice potential safety issues.
The medical field is constantly evolving, making it essential for healthcare professionals to stay current. Continuous learning helps clinicians keep abreast with new treatments, emerging technologies, malpractice regulations, and best practices in risk management.
Regular in-practice simulations and workshops enable staff to practice complex procedures and emergency scenarios in a safe, controlled environment. Analyzing past incidents and near-misses helps identify gaps, refine protocols, and prevent repeated errors. Ensure all team members actively participate in risk management programs that cover critical topics such as legal updates, compliance requirements, patient communication, and teamwork strategies.
Encouraging continuous learning fosters a learning culture in which staff feel empowered to raise concerns, share insights, and implement best practices.
Technology is a game-changer, streamlining tedious tasks that once led to errors, patient frustration, and liability exposure.
Leveraging the right tools significantly reduces risk and elevates care quality. Consider adopting the following:
Early recognition of warning signs in patients is a decisive strategy for reducing malpractice exposure. Recognizing patients who may likely pursue a claim allows your practice to take preventive steps. Some characteristics of a potentially litigious patient include:
By spotting these warning signs early, you can proactively address concerns, clarify expectations, document interactions carefully, and maintain open communication, ultimately reducing the likelihood of a malpractice claim.
Even with the best precautions, no practice is completely immune to risk. Comprehensive malpractice insurance is vital to safeguard your practice and protect against financial losses.
When selecting coverage, consider:
Review and update your policy as your practice grows or adds new services. Investing in the right coverage protects your finances and offers peace of mind, allowing you to focus on delivering care.
Malpractice risk can never be fully eliminated, but with the right strategies, your practice can mitigate the risk. By instilling a culture that prioritizes safety and clear communication, leverages technology, and maintains robust documentation, you establish robust malpractice protection.
Schedule a Free Consultation!
