Private practice is fading, or so the story goes.
Yet despite the popular narrative, more than half of U.S. physicians still choose to work independently, proving their resilience and reaffirming their vital role in patient-centered care.
Running a private medical practice, however, is no easy ride. You’re at the wheel, navigating potholes, inching through traffic jams, and constantly adjusting your route to keep moving forward. Between patient care, paperwork, staffing challenges, and financial pressures, the road can feel rough.
But it’s worth every mile. Because in private practice, you have something few others do: the autonomy to chart your own path, make a meaningful difference, and put quality care above all else.
Join us as we explore four common challenges private practices face today, and the smart, practical strategies that can help you navigate them with clarity and confidence.
Administrative workload remains one of the biggest pain points for physicians in private practice. A recent MedCentral survey found that 66% of physicians consider administrative work the most challenging aspect of running an independent practice. These non-clinical responsibilities eat into valuable time that could be devoted to patient care, and they’re a leading driver of physician burnout.
While burnout rates have dropped since the pandemic, they remain concerning; 43.2% of physicians report experiencing at least one symptom of burnout.
Fortunately, automation can shoulder much of this administrative burden, freeing up physicians. And you don’t need to overhaul your entire system to see results; most EHR platforms already include built-in automation features that most practices overlook. Leveraging these can streamline tasks such as appointment reminders, documentation templates, and claims management.
Another common hurdle to streamlining administrative tasks is legacy software that does not support newer updates or integrate with advanced features. Regularly reviewing your tech stack and updating outdated systems can prevent inefficiencies and improve productivity.
Furthermore, incorporate AI-based solutions to achieve greater operational precision and efficiency.
Some impactful options include:
Adopting the right technology transforms workflows, improves team productivity, and ensures your practice thrives.
A single misstep in technology adoption can derail your finances and disrupt operations. Choosing a poor-fit system or rushing through implementation often creates more work than less.
The goal is simple: adopt technology that alleviates pain, not adds to it.
The healthcare tech market is crowded with options, but not every solution will fit your practice’s needs. Each practice is unique: in the services it offers, the challenges it faces, and the goals it strives to achieve. Selecting the right technology is just as important as integrating it successfully.
As you narrow down your options, weigh each solution against the following benchmarks:
Technology should reduce burnout, not add to it. A lengthy or complicated onboarding process can overwhelm physicians and staff, delaying productivity. Choose systems with guided setup, role-based training, and responsive vendor support that help your team get up to speed quickly, without disrupting patient schedules or daily workflows. Remember, the smoother the onboarding, the faster you realize ROI.
A full-scale system overhaul can drain financial resources. Instead, opt for phased implementation, roll out one module or department at a time. This approach minimizes downtime, spreads costs over time, and helps you evaluate usability, workflow compatibility, and ROI before expanding across the practice.
It also allows your team to adapt gradually, ensuring that lessons learned during the pilot stage inform the next phase of integration.
The whole point of technology is to simplify tasks. A complex EHR system that demands multiple clicks for every entry only worsens frustration. Look for solutions with intuitive interfaces, customizable templates, and voice or AI-assisted documentation.
Ease of use is fundamental to successful adoption. A system that feels intuitive encourages consistent, accurate use, boosting efficiency and care quality.
Long-term vendor lock-ins can become costly mistakes if the system doesn’t meet expectations. Seek contracts with clear service-level agreements (SLAs), transparent pricing, and easy exit or upgrade options. A vendor confident in their product will give you flexibility.
Avoid being tied down by multi-year commitments; instead, choose solutions that allow scalability, periodic reassessment, and freedom to pivot as your practice grows or needs change.
Your staff are the end users; their input is invaluable. Involve them early in demos, pilot testing, and decision-making. Their day-to-day experience provides insight into what works and what doesn’t.
Gather feedback not just from clinical staff but also from front-desk teams and billing personnel, who often bear the brunt of inefficiencies. Engaging your staff fosters buy-in, smoother transitions, and a higher success rate.
The best technology doesn’t work in isolation. Ensure the system integrates seamlessly with your existing EHR, billing, telehealth, and analytics tools. Poor interoperability creates data silos, duplicative work, and reporting gaps. Look for solutions that support HL7/FHIR standards and are compatible with your existing software ecosystem.
Technology is never “set and forget.” Choose vendors that offer continuous technical support, regular updates, and training resources. This ensures your staff stays confident using new features and that your system evolves alongside your practice’s needs.
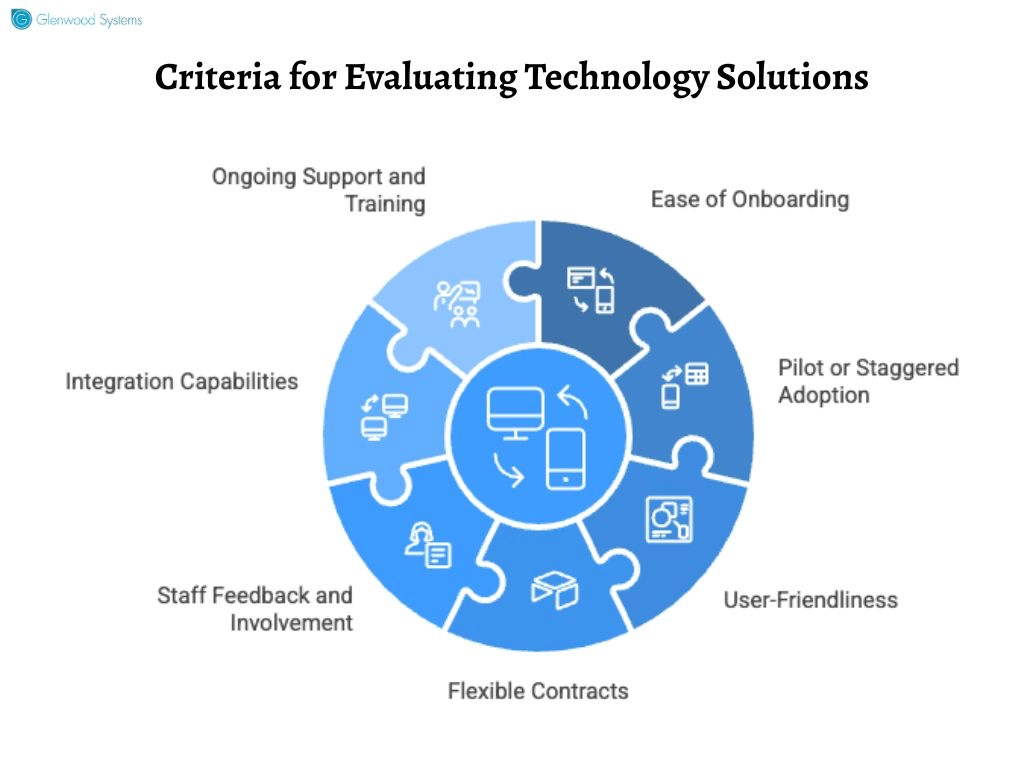
Choosing the Right Practice Systems
Cash flow keeps every business running, and medical practices are no different. Each delayed payment or denied claim creates a ripple effect that disrupts financial stability and creates operational bottlenecks that directly affect patient care.
Reimbursement challenges are growing more complex as payers tighten prior authorization rules, delay claim approvals, and increase scrutiny on medical necessity. It’s no surprise that it ranks as the second most common challenge in private practice; a reality acknowledged by nearly six in ten physicians. Independent and small-group practices, in particular, bear the brunt, often lacking the negotiating power to secure fair reimbursement. The result? More time spent on administrative back-and-forth and less on patient care.
Here’s a proactive approach to ensure your practice remains financially stable and maintains a predictable revenue stream.
Financial sustainability in private practice is achieved by mastering the financial workflows that support it.
Staffing constraints have become a major operational hurdle in healthcare. High turnover, coupled with a competitive talent market, has made recruitment increasingly difficult. With healthcare staffing shortages at critical levels, private practices, often operating with limited resources, struggle to compete with larger health systems offering higher pay and extensive benefits.
The most effective strategy isn’t just hiring new staff but retaining the team you already have. Practices that invest in employee satisfaction, fair compensation, flexible scheduling, and professional development often see lower turnover and stronger patient relationships. According to Gallup, organizations that prioritize employee engagement experience 21% lower turnover rates and 14% more productivity.
Additionally, Non-Physician Providers (NPPs) such as Nurse Practitioners (NPs) and Physician Assistants (PAs) are invaluable in bridging care gaps and mitigating workforce shortages. They bring specialized expertise, improve access, and help practices expand their service capacity without overburdening physicians. Today, 56% of healthcare organizations leverage NPPs to enhance efficiency. Integrating NPPs effectively through clear role definitions, team-based models, and mentorship programs helps sustain operations, reduce wait times, and elevate quality care delivery.
Challenges are part of every meaningful pursuit. What defines success is the ability to turn those challenges into catalysts for progress.
At Glenwood Systems, we empower private practices to overcome healthcare challenges and achieve their goals. Our intelligent practice management solutions (GlaceEMR, GlaceRCM, GlaceScribe, and more) streamline operations, reduce administrative load, and ensure seamless regulatory compliance. With the power of AI, automation, data-driven insights, and dedicated support, Glenwood helps you work smarter, improve efficiency, and achieve sustainable success.
Schedule a Free Consultation!
